Seng J, Cai M, Oka P (December 27, 2025) Cureus 17(12): e100214. doi:10.7759/cureus.100214
Abstract
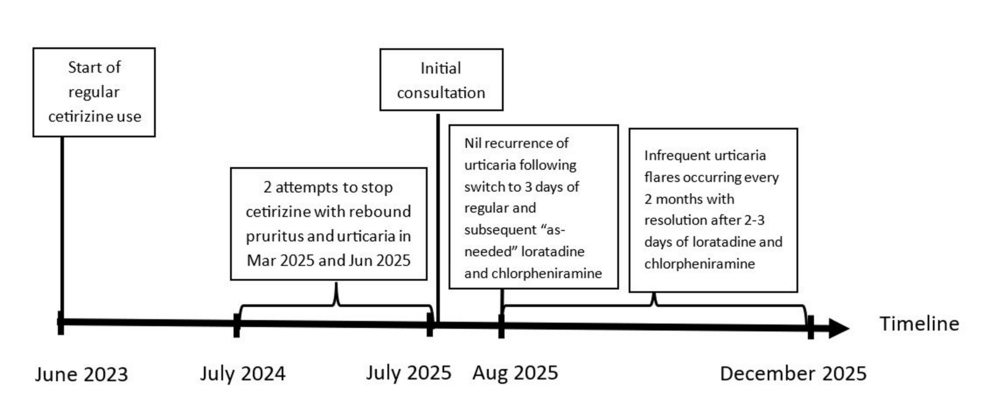 |
| Timeline of events |
A blog that publishes updates and open access scientific papers about allergy, asthma and immunology. Editor: Juan Carlos Ivancevich, MD. Specialist in Allergy & Immunology
Seng J, Cai M, Oka P (December 27, 2025) Cureus 17(12): e100214. doi:10.7759/cureus.100214
Abstract
 |
| Timeline of events |
Preface
We are pleased to welcome all participants to the 14th C1-inhibitor Deficiency & Angioedema Workshop.
The aim of the Workshop is to present new research findings related to rare bradykinin-mediated angioedema disorders. These include conditions caused by hereditary or acquired C1-inhibitor deficiency, as well as those with a hereditary background but normal C1-inhibitor levels. This year, a record number of abstracts will be presented over the four-day program, including 49 oral and 58 poster presentations. In addition to previously unpublished findings, five outstanding keynote lectures will also be delivered.
On the opening afternoon, Nobel Laureate Katalin Karikó will give a special lecture on the development of the mRNA vaccine, sharing all the insights gained from the long and persistent journey that led to the production of life-saving mRNA-based vaccines.
Semenzato L, Le Vu S, Botton J, et al. JAMA Netw Open. 2025;8(12):e2546822. doi:10.1001/jamanetworkopen.2025.4682
Question Are COVID-19 mRNA vaccines associated with the long-term risk of all-cause mortality?
Findings In this cohort study including 22.7 million vaccinated individuals and 5.9 million unvaccinated individuals, vaccinated individuals had a 74% lower risk of death from severe COVID-19 and no increased risk of all-cause mortality over a median follow-up of 45 months.
Meaning These national-level results found no increased risk of 4-year all-cause mortality in individuals aged 18 to 59 years vaccinated against COVID-19, further supporting the safety of the mRNA vaccines that are being widely used worldwide.
Importance While several studies have assessed the impact of COVID-19 vaccination on short-term mortality, none have compared long-term mortality by vaccination status, particularly in young individuals who are less likely to experience severe disease following SARS-CoV-2 infection.
Ali, A., Alamri, A., Mishra, V.K. et al. BMC Immunol (2026). https://doi.org/10.1186/s12865-025-00795-4
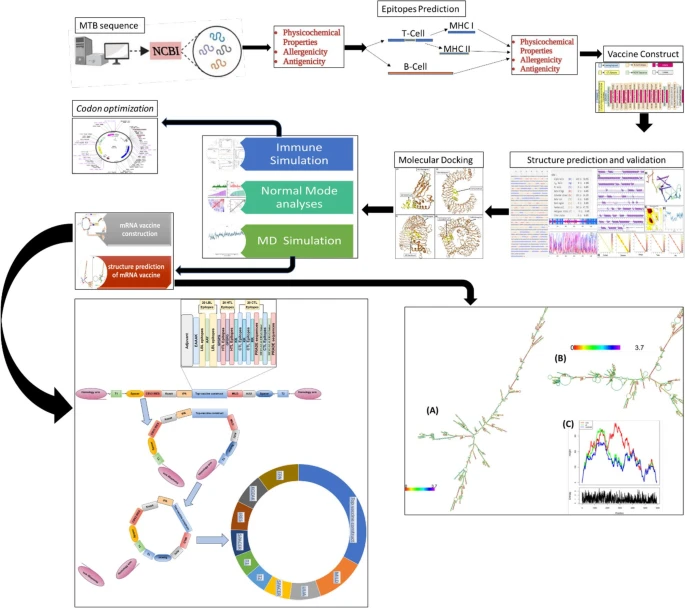 |
| Graphical Abstract |
 |
| Visual Summary |
Aparicio E E, Guerrero D V, Alcántara V D, et al. (December 26, 2025) Cureus 17(12): e100143. doi:10.7759/cureus.100143
Abstract
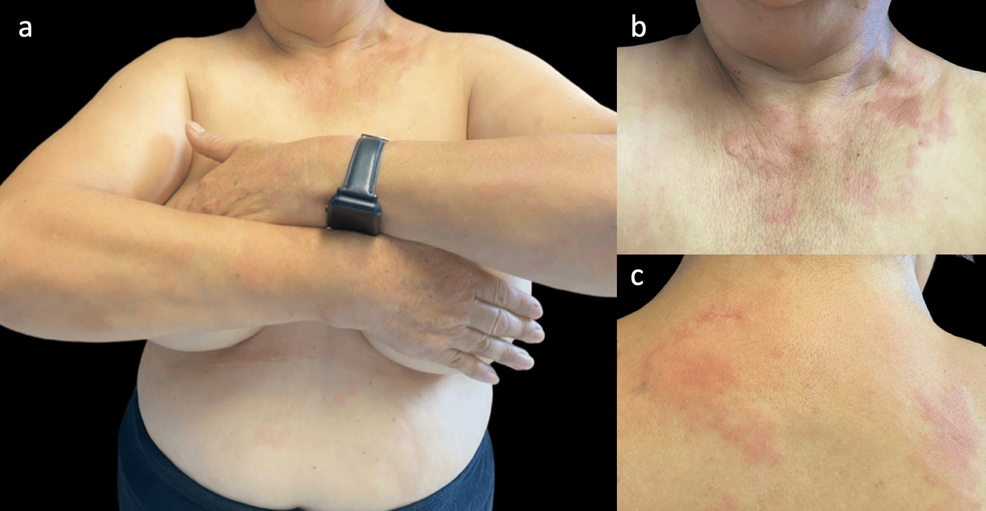 |
| Cutaneous manifestations of hypocomplementemic urticarial vasculitis |
Rossi CM, Terreehorst I, Apostolidou E et al. Allergy. 2025 Dec 16. doi: 10.1111/all.70183.
ABSTRACT
 |
| Risk of bias (RoB) domains for the randomized controlled trials (RCT) on the development of eosinophilic esophagitis (EoE) after allergen immunotherapy (AIT). |
Singh AK, Shaili S, Siddiqui A et al. Front Allergy. 2025 Dec 4;6:1636415. doi: 10.3389/falgy.2025.1636415.
Abstract
Allergic rhinitis (AR) is a complex, multifactorial condition that continues to pose significant clinical and public health challenges, despite the availability of established therapeutic strategies. It significantly contributes to a lower quality of life by causing sleep issues, mental fatigue, and a decline in productivity. A thorough grasp of AR is crucial to enhancing diagnosis and treatment results because of its pervasive effects and ongoing management gaps. This review covers a wide range of topics, such as classification schemes, historical perception, and physical consequences of AR.